A review article survey by Dental Implants Melbourne suggests that iron deficiency anemia and severe tooth rot are linked. Although both illnesses are connected with poor diets and are more frequent in those living in poverty areas and with underlying medical issues, it is uncertain if the link is correlative or causal.
According to new study from the University of Pennsylvania and Indiana University, an FDA-approved medication for iron deficiency anemia might potentially be used to cure, prevent, and even diagnose tooth disease. The treatment, a mixture of an iron-oxide nanoparticle-containing solution termed ferumoxytol and hydrogen peroxide, was applied to actual tooth enamel and worn by research participants in a denture-like prosthesis.
The research, which was published in the journal Nano Letters, discovered that using ferumoxytol twice a day, which activated hydrogen peroxide in a follow-up rinse, decreased the formation of dangerous dental plaque and had a focused effect on the bacteria that cause tooth decay. Nanoparticles with enzyme-like capabilities are frequently referred to as “nanozymes,” and their potential in biological and environmental applications is rapidly being investigated.
Hyun (Michel) Koo, a professor at the University of Pennsylvania School of Dental Medicine, states, “We discovered that this strategy is both exact and successful.” “It decreased the degree of enamel erosion by disrupting biofilms, notably those generated by Streptococcus mutans, which cause caries. This is the first research we’re aware of that shows nanozymes have therapeutic benefit against an infectious condition in a clinical environment.”
The study builds on a paper published in Nature Communications in 2018, in which Koo and colleagues, including David Cormode of Penn’s Perelman School of Medicine, demonstrated that an iron oxide nanoparticle-hydrogen peroxide treatment could prevent biofilm accumulation and tooth decay in both an experimental and animal model.
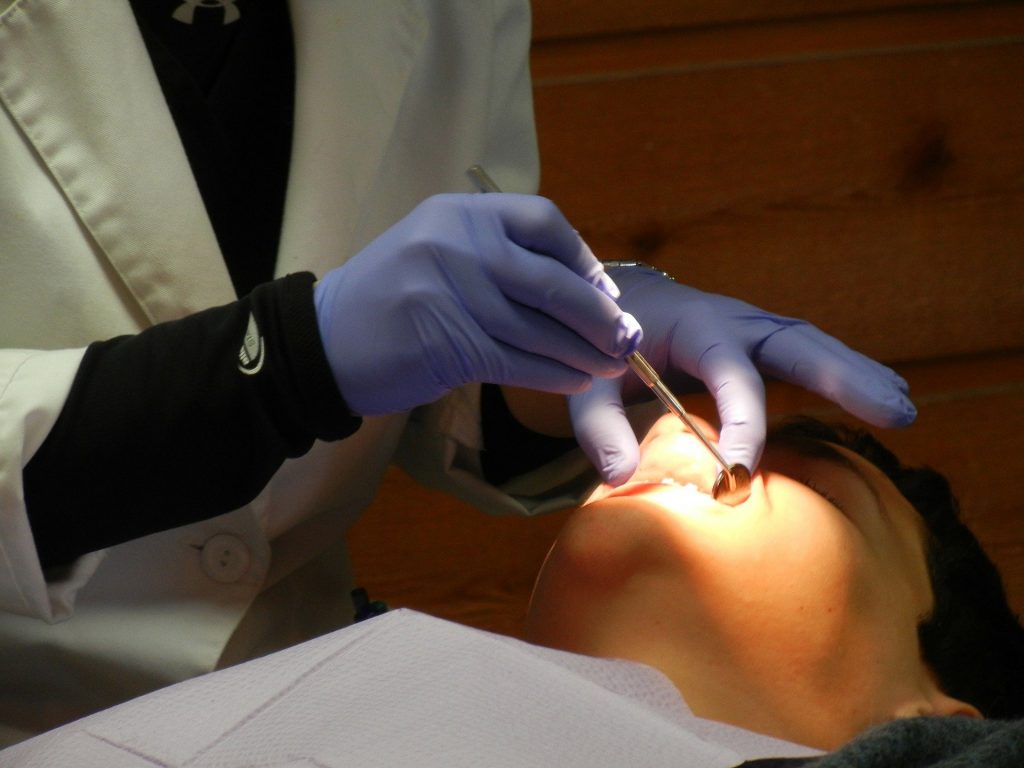
The scientists intended to take the next logical step in their research by working with humans. They used a detachable, denture-like prosthesis with genuine tooth enamel affixed to 15 people in a randomized research, a technology invented and thoroughly tested by Domenick T. Zero of Indiana University, a co-corresponding author on the present publication.
Four times a day, research participants applied a sugar-containing solution to the device, simulating high-sugar meals and snacks taken in regular life. Instead of brushing the enamel sample, participants were instructed to rinse the gadget twice a day. Participants were placed into three groups: one that received ferumoxytol followed by a hydrogen peroxide rinse, another that received a solution containing the inactive chemicals in ferumoxytol, and a third that received only water.
The researchers examined the biofilms that had formed on the enamel specimens after 14 days. They discovered that the experimental treatment effectively slowed the formation of S. mutans biofilms and killed the bacteria with great specificity. The ferumoxytol-hydrogen peroxide treatment had no effect on other commensal bacteria identified in the mouth.
Previous research has demonstrated that iron oxide nanoparticles do not adhere to mucosal tissue in the mouth and do not produce cytotoxicity or changes in the oral microbiota in an animal model, indicating that the method is safe.
“It doesn’t appear that this therapy has any detrimental or off-target consequences,” Koo adds.
There are three reasons for this accuracy. Only a very acidic environment, such as that which exists when caries-causing bacteria are present and active, can catalyze hydrogen peroxide. The therapy also causes the biofilm’s sticky carbohydrate matrix to break down, exposing the microorganisms and dissolving the biofilm. Ferumoxytol can also attach to receptors on the cell membrane of S. mutans, making it easier to kill it.
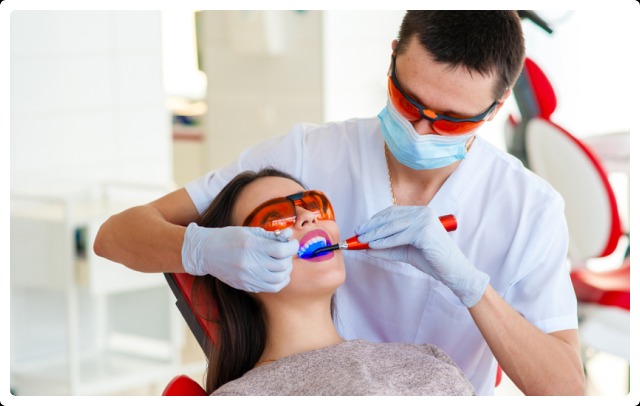
The researchers added a marker that becomes blue when exposed to reactive oxygen species, such as those produced by ferumoxytol nanoparticles catalyzing hydrogen peroxide catalysis. The degree of blue labeling did, in fact, correspond to acidic biofilms harboring S. mutans, according to the Dental Implants Melbourne researchers.